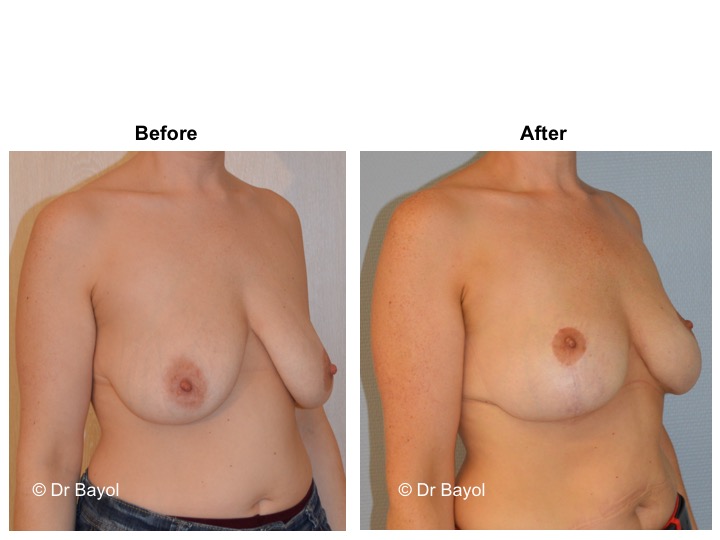
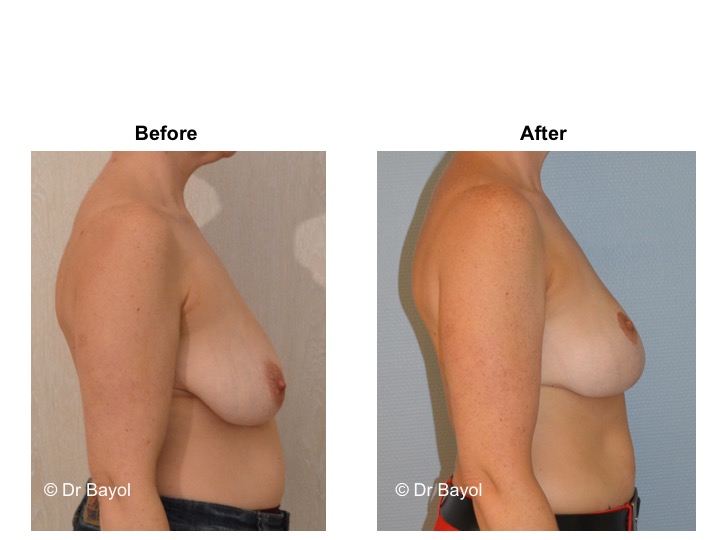
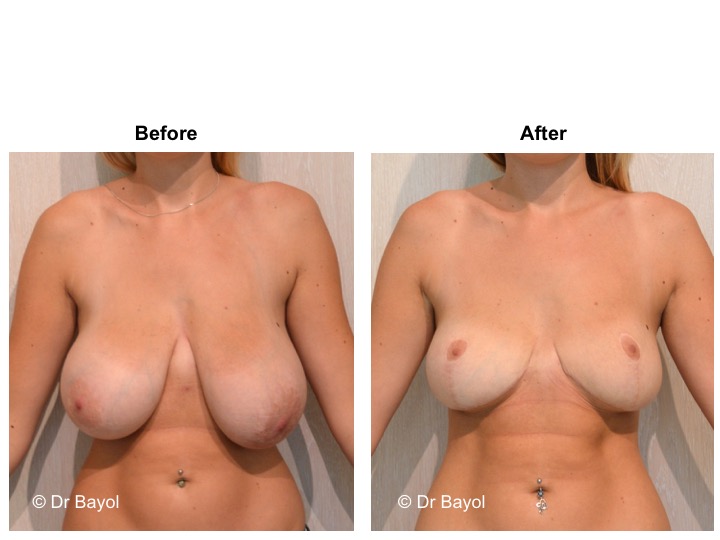
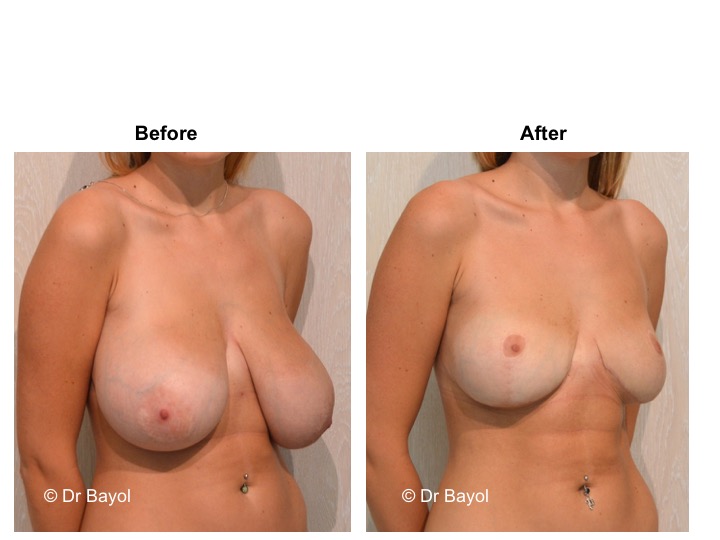
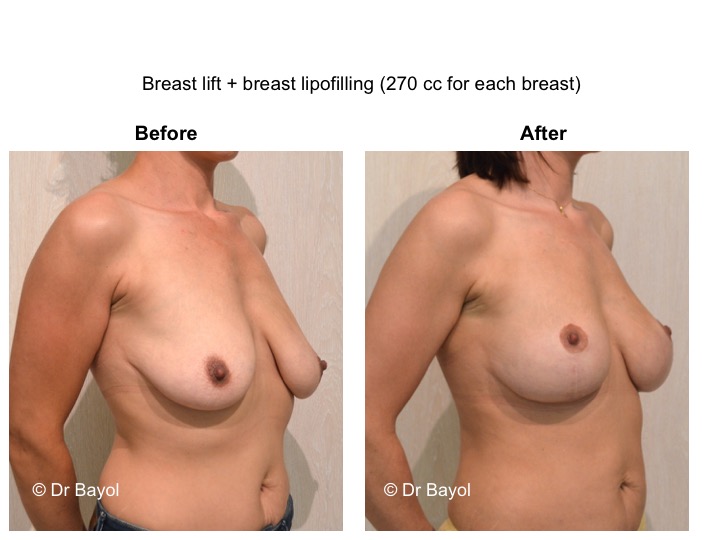
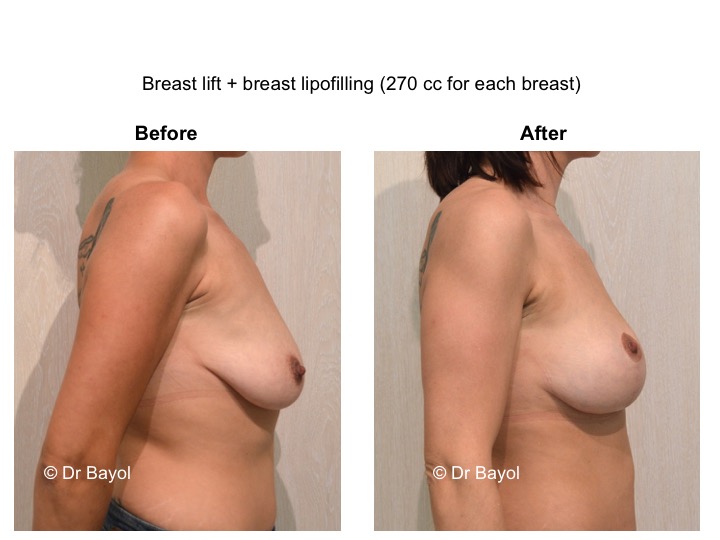
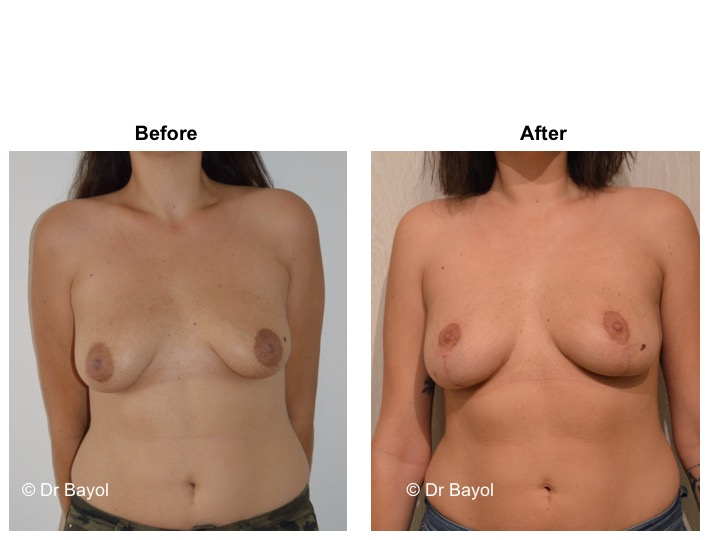
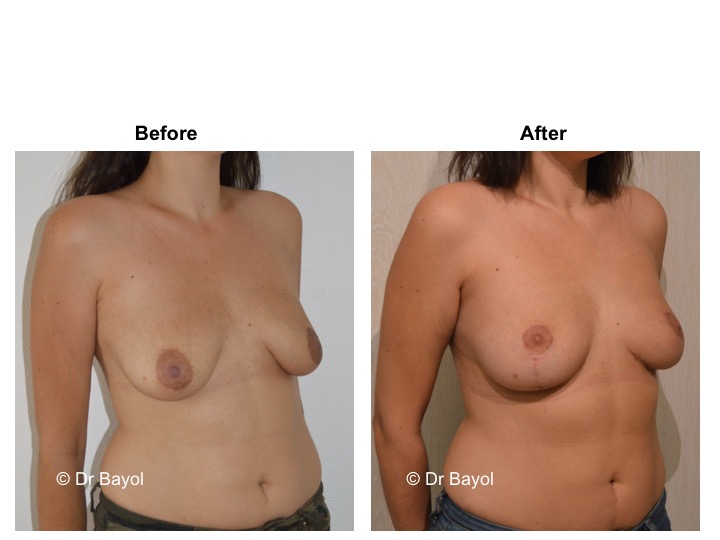
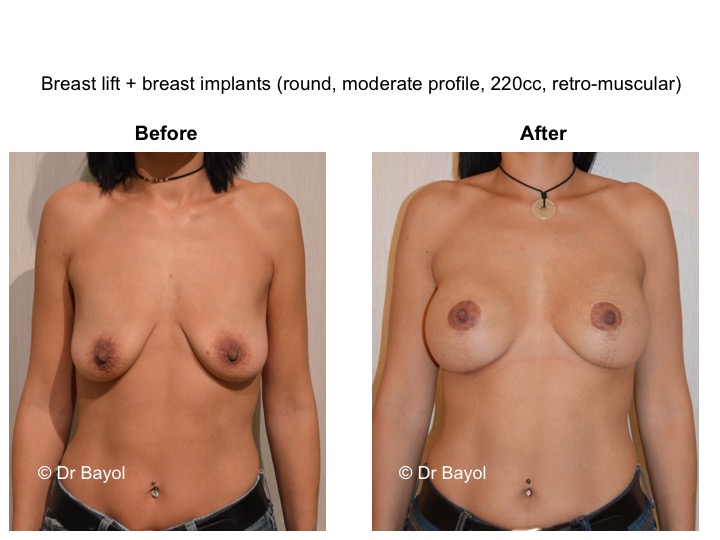
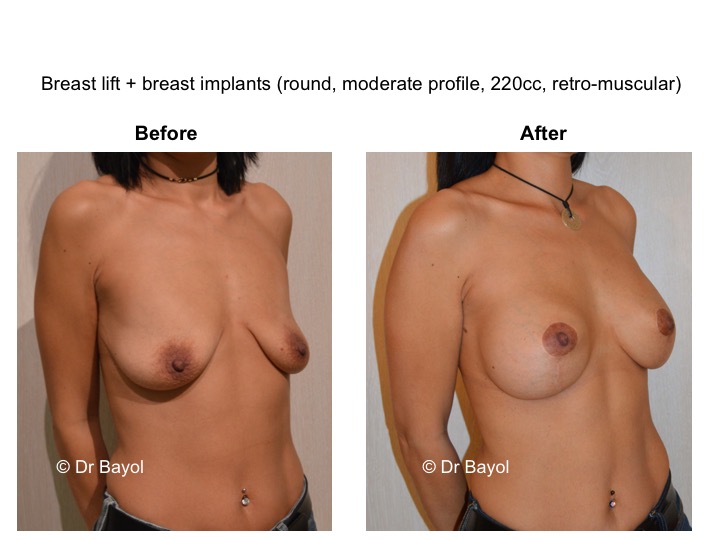
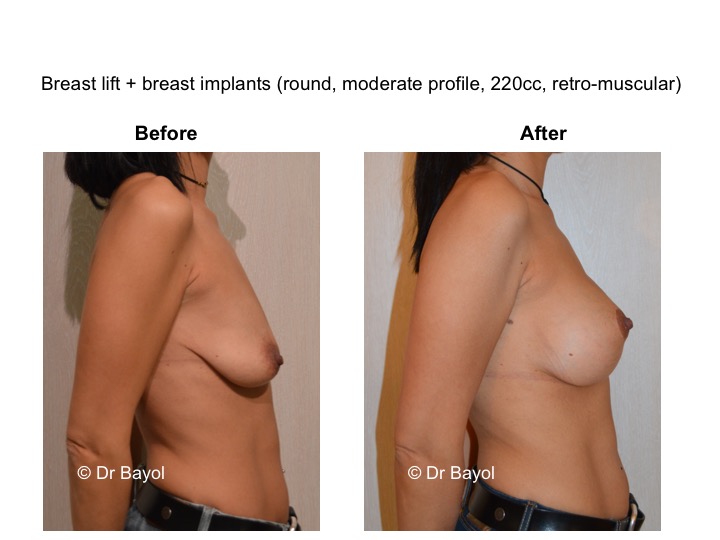
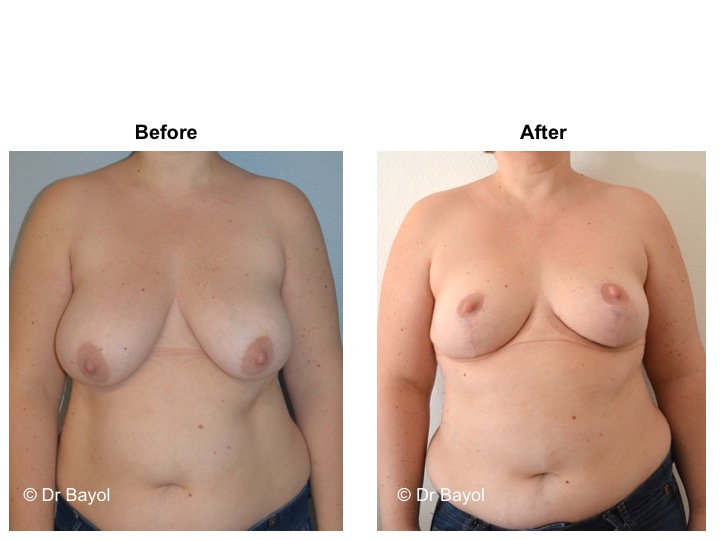
MAMMARY PTOSIS OR BREAST LIFTING
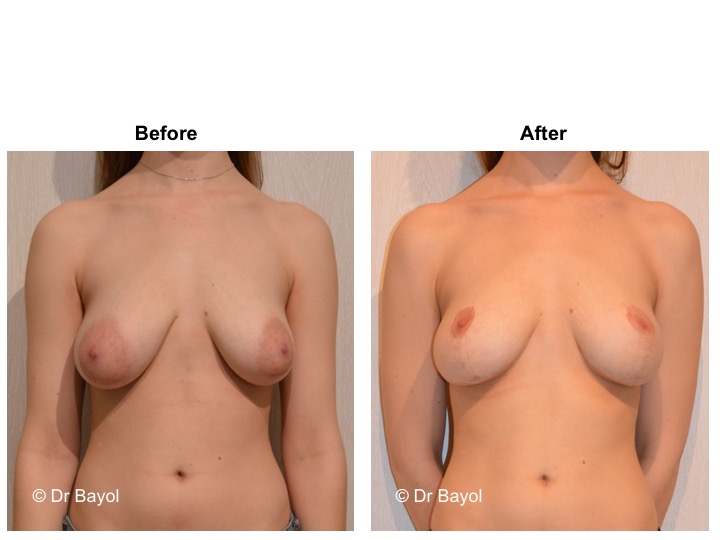
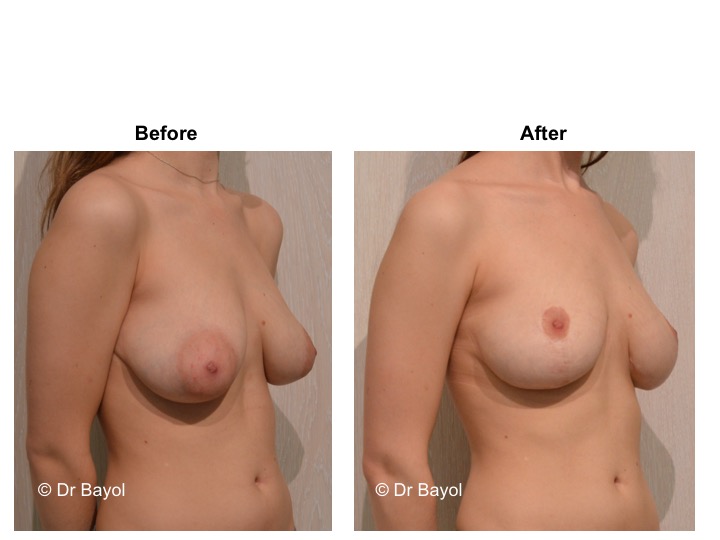
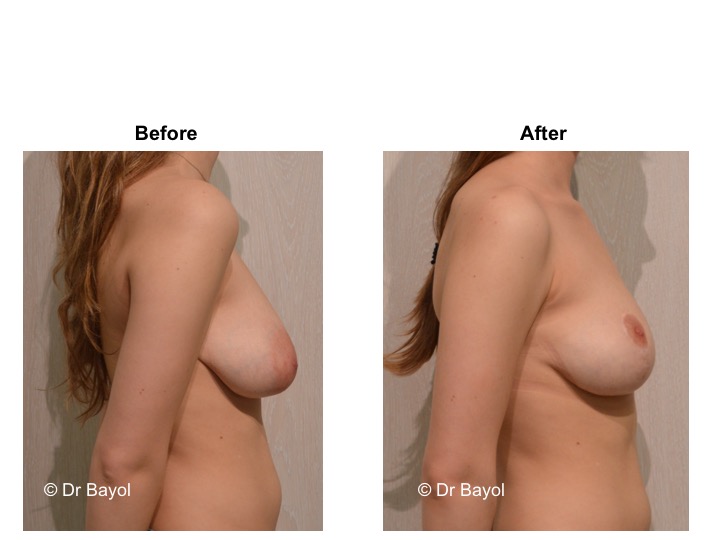
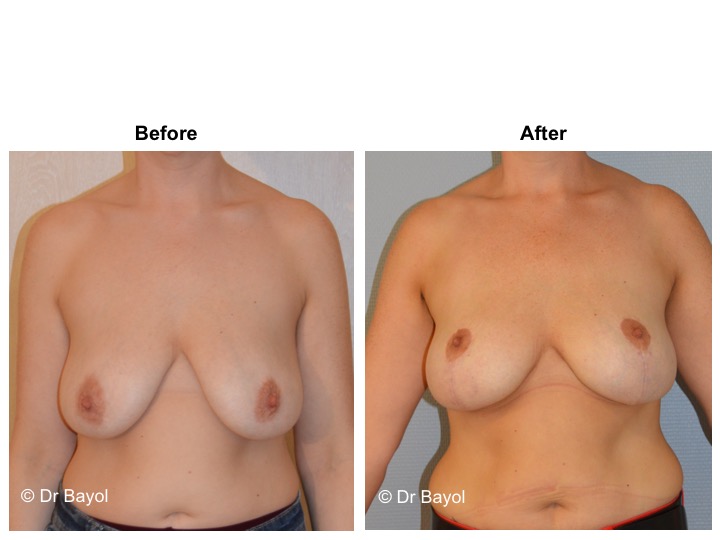
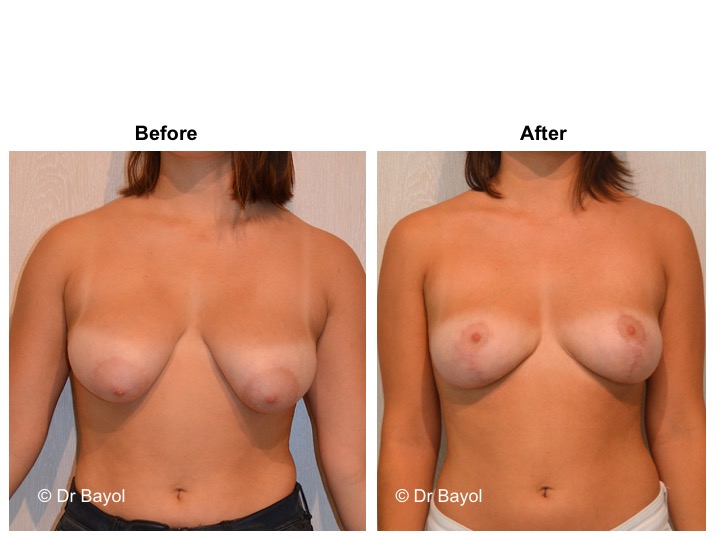
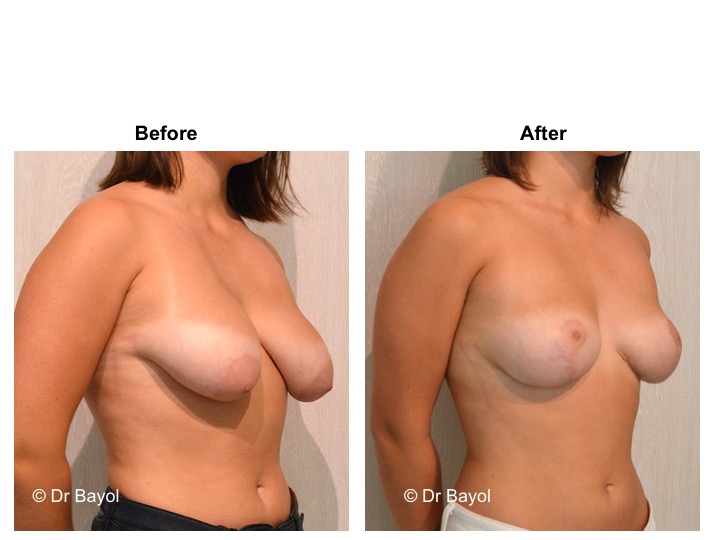
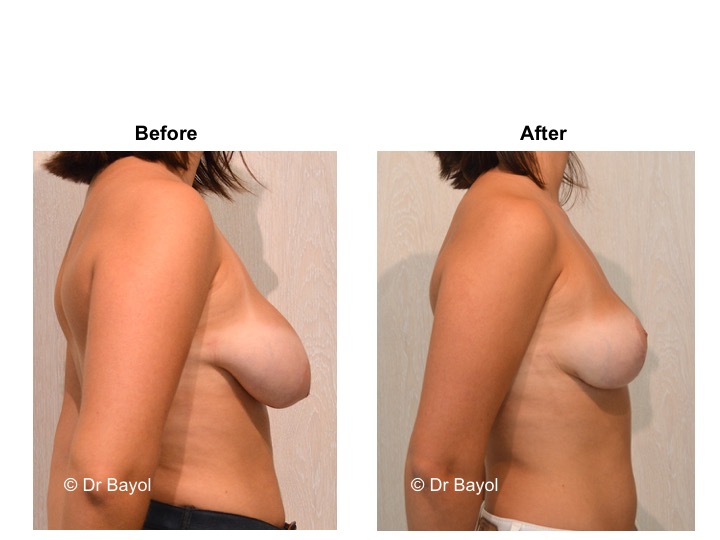
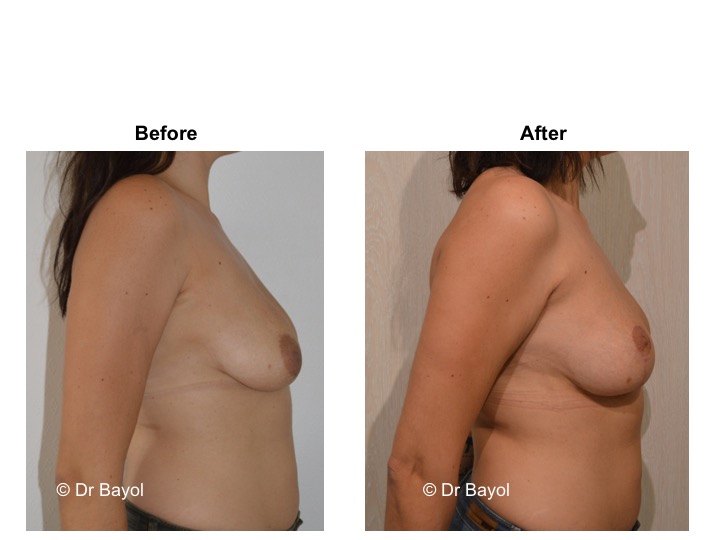
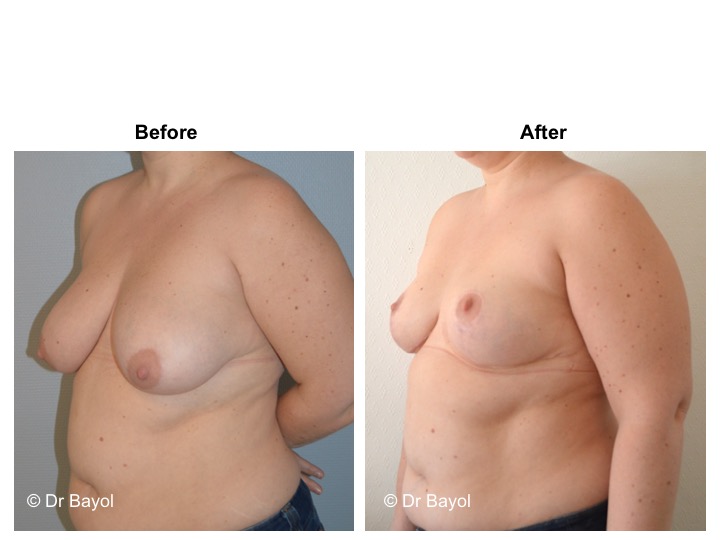
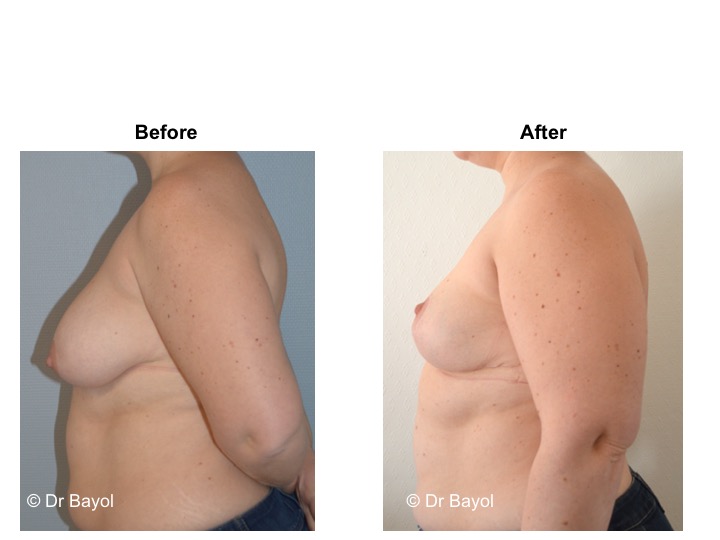
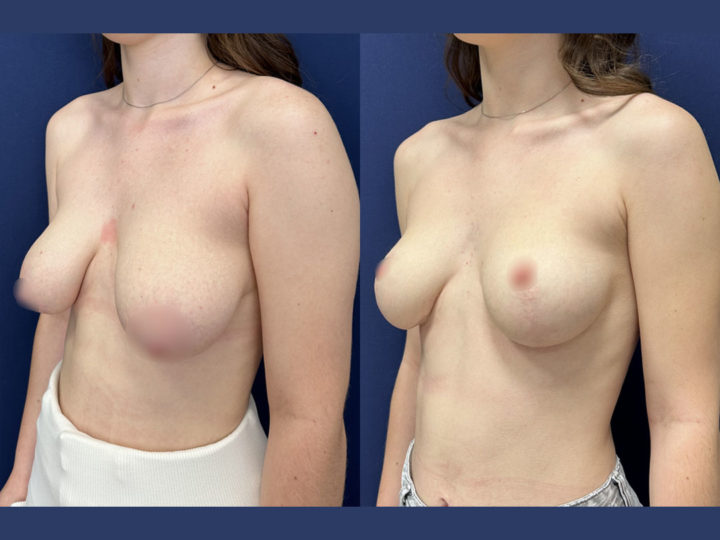
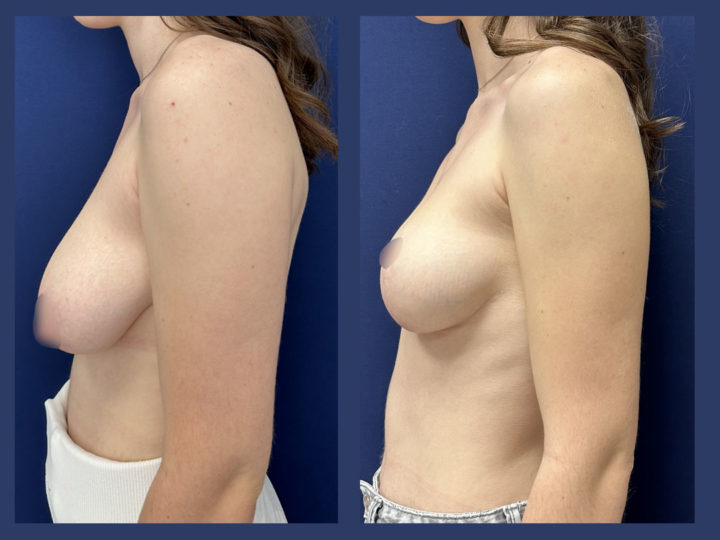
Because it can reshape the breast and give it volume, with or without implant, this procedure is particularly suitable for women hampered by the effects of time on their breasts. After surgery, breasts regain their former shape and keep a completely natural aspect.
> all about MAMMARY PTOSIS, BREAST LIFT AND MASTOPEXY <
COSMETIC SURGERY FOR MAMMARY REPOSITIONING OR BREAST LIFTING IN MONTREUX, LAUSANNE AND GENEVA (SWITZERLAND)
Mammary ptosis is defined by a collapse of the gland and a distension of the skin that envelops it. The breast is in a too low position and frequently “hollow“ in its upper part.
Breast ptosis may naturally occur but most often appears after a significant weight loss or after breastfeeding.
It can be isolated: it is then called pure ptosis. It can also be associated with a certain degree of breast hypertrophy (lien vers “hypertrophie mammaire”).
Mammary ptosis can also be observed in the case of a breast that is too small (hypoplasia or mammary hypotrophy).
OBJECTIVES OF THE MAMMARY PTOSIS TREATMENT
The aim of the surgery is to put the areola and the nipple in a proper position, to re-concentrate and to ascend the gland. It will also allow to remove the excess skin in order to obtain two harmonious breasts, nicely curved and ascended. It is a true lifting of the breast.
PRINCIPLES OF BREAST LIFTING
The procedure aims to reposition the areola and reshape the breast by focusing on the cutaneous envelope and on the glandular tissue. The gland is concentrated and placed in a proper position.
- To reposition the areola:
The areola is normally located 17 to 19 cm from the clavicle, 9 to 10 cm from the midline, and 4 to 6 cm from the fold under the breast. The cosmetic surgeon will draw a cutting pattern on both breasts before the surgical procedure with the position of the future areola and the excess skin that will have to be removed (Figure 1).
Figure 1: Ideal position of the aerola and preoperative drawing
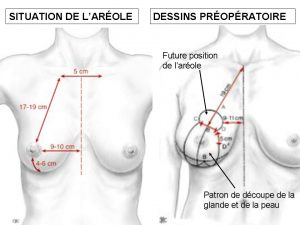
After having created a shred in the mammary gland the first stage of surgery involves ascending the areola and reducing its diameter if it is distended (Figure 2).
Figure 2: Repositioning of the aerola and reduction of its diameter
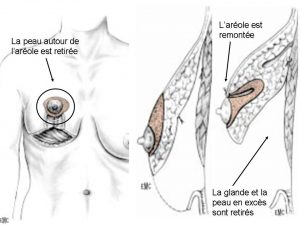
-To remodel the mammary gland and remove the excess skin:
After ascending the areola, the residual glandular volume is ascended, concentrated and remodeled in harmony with the silhouette of the patient and according to her desires.
It is then necessary to adapt the skin envelope, which requires removing the excess skin in order to ensure a good hold and a beautiful shape to the new breast. The edges of the skin which have been cut are sutured at the end of the surgery: these sutures are at the origin of the scars.
In the case of a very large ptosis, the scar has the shape of an inverted T with three components (figure 3): around the areola between the brown skin and the white skin (peri-areolar), vertical between the lower areola and the mammary fold, horizontal concealed in the fold under the breast. The length of the horizontal scar is proportional to the size of the ptosis. However, this scar is shorter compared to the case of a mammary breast reduction for hypertrophy (lien vers “hypertrophie mammaire”).
Figure 3: Inversed T shaped scar
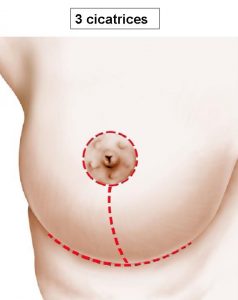
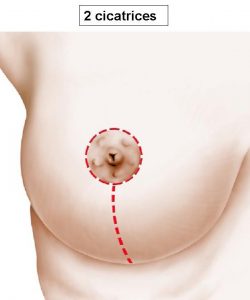
Sometimes, in the presence of a moderate breast ptosis, a “vertical” method can be performed (Figure 4) which allows to eliminate the transverse scar in the fold under the breast and to reduce the scarring to its peri-areolar and vertical components.
In some cases of very moderate mammary ptosis, it is possible to use a technique that allows correction of the sagging only with a scar positioned around the areola (Figure 5). This method is called “round block”.
Figure 5: peri-areolar or « round block » scar
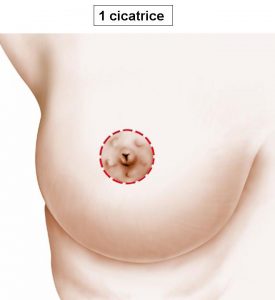
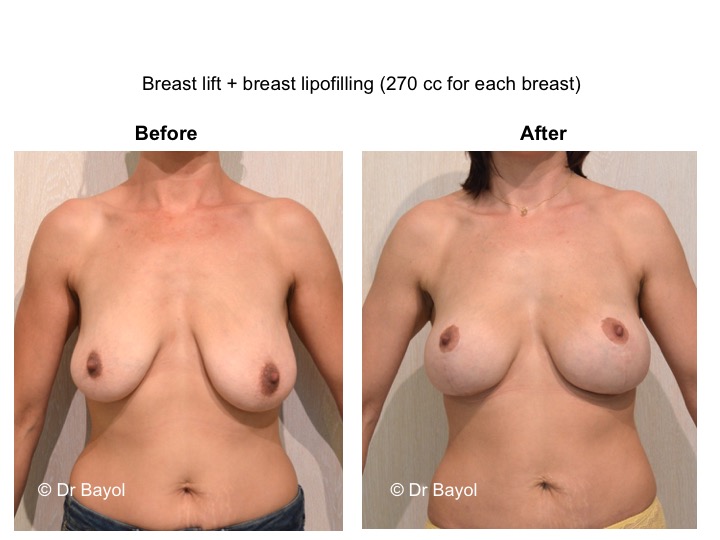
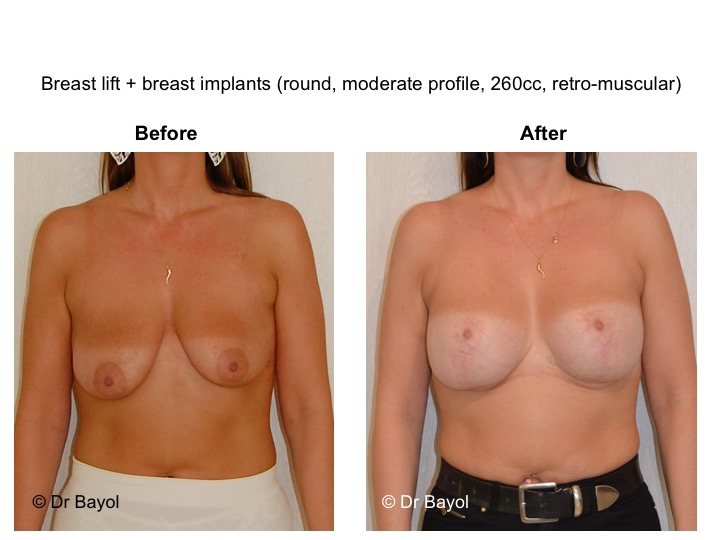
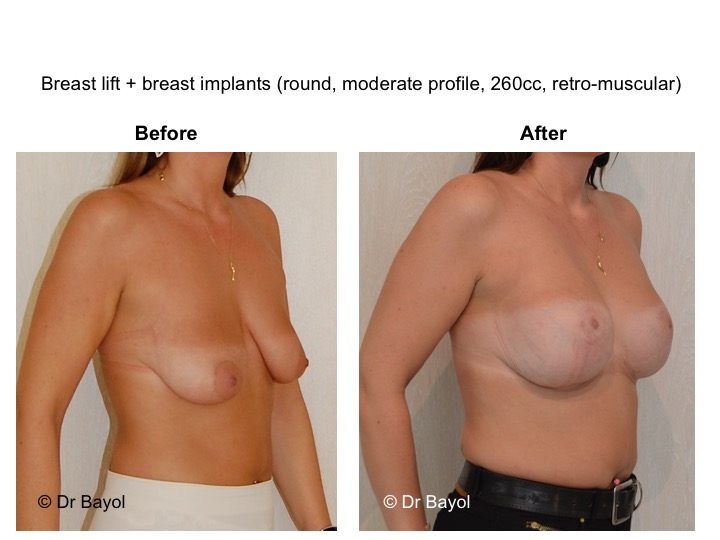
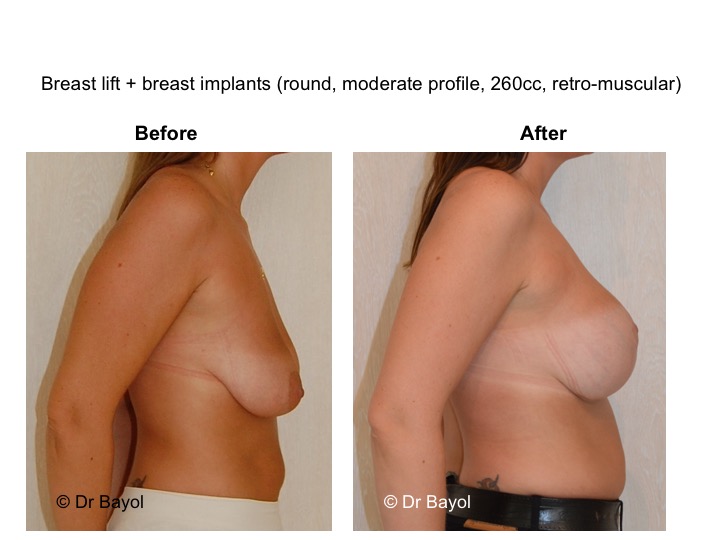
Finally, when ptosis is associated with an insufficient volume (mammary hypotrophy), it may be preferable to set up breast implant during the same surgical procedure in order to restore a satisfactory volume (lien vers “prothèse mammaire”).
Cosmetic surgery of the breast ptosis can be performed from the end of growth and beyond, throughout the patient’s lifetime.
A later pregnancy is of course possible as well as breastfeeding, but it is advisable to wait at least six months after the surgery.
The risk of developing cancer is not increased by this intervention.
BEFORE THE SURGICAL PROCEDURE
Doctor Jean-Charles BAYOL welcomes you at Laclinic-Montreux (near Sion and Fribourg), or at the Beauty Suite in Lausanne, (only 30 minutes from Genevaand Neuchâtel).
A usual preoperative assessment is performed according to the prescriptions.
The consultation with the anesthesiologist will happen no later than 48 hours before surgery.
In addition to the usual preoperative examinations, a radiological assessment of the breast will be prescribed (mammography and ultrasound).
To refrain from smoking is strongly recommended, at least one month before and one month after surgery, as tobacco consumption may delay the healing process.
Stopping oral contraception may be required, especially if there is an associated risk (obesity, poor venous condition, bleeding disorder).
Medicine containing aspirin should be prohibited within 10 days before surgery.
TYPE OF ANESTHESIA AND HOSPITALIZATION MODALITIES
This procedure will be performed under anesthesia in the operating room, during which you will be deeply asleep.
A hospitalization of one to two days is usually required at Laclinic in Montreux.
THE SURGICAL PROCEDURE
Each cosmetic surgeon has his own technique and adapts it to each case in order to obtain the best result. However, common basic principles can be explained:
- The Glandular tissue that has been removed, is systematically sent to a specialized laboratory for a microscopic examination (histological examination).
- At the end of the procedure, a modeling dressing is made with elastic bands in the form of a bra.
- Depending on the surgeon, the importance of hypertrophy and the placement of the breast implants, the procedure can last from two to four hours.
AFTER THE INTERVENTION, POSTOPERATIVE FOLLOW-UPS
The postoperative follow-ups are generally painless, requiring only simple analgesics.
Swelling (edema) and bruising of the breast, as well as discomfort when elevating the arm, are commonly observed.
In order to reduce bruises and swelling as quickly as possible, you will be systematically taken care of by the physiotherapy department for postoperative care. The day following surgery, gentle massages of the operated area and LED care will ensure lymphatic drainage and will promote the healing process. Several weeks after the procedure, a LPG treatment can be undertaken.
The first dressing will be removed after 24 hours and replaced by a lighter dressing. Then, we will put in place a bra without armature, ensuring a good restraint. The wearing of this bra is advised for about two months, night and day, after surgery.
The check-out will take place one to two days after the procedure.
The sutures, if not resorbable, will be removed between the eighth and fifteenth day after surgery.
A period of convalescence of 8 to 15 days should be scheduled.
It is advised to wait one to two months to resume a sporting activity.
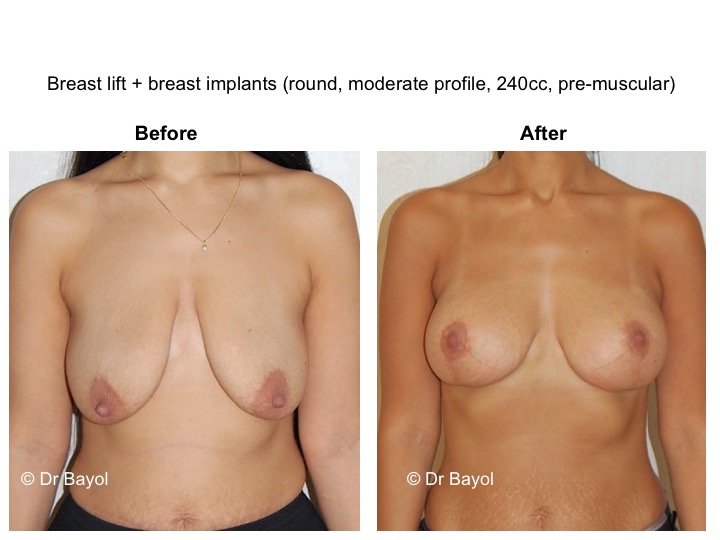
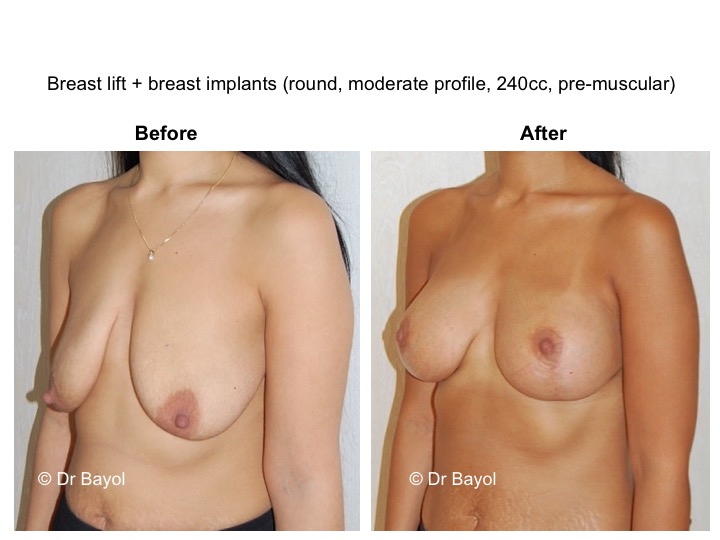
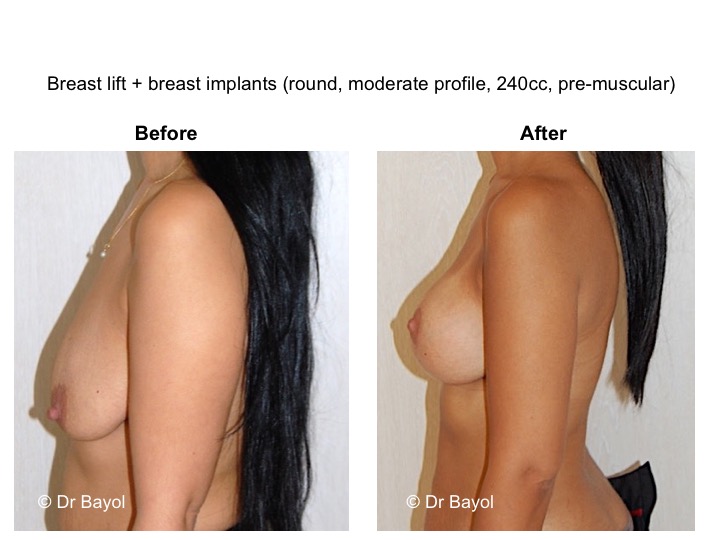
THE RESULT OF MASTOPEXY OR BREAST LIFTING IN MONTREUX, LAUSANNE AND GENEVA (SWITZERLAND)
It cannot be judged until the sixth month after the procedure. After this period the breast will most likely have a harmonious and natural curve, symmetrical or very close to symmetry. Beyond the local improvement, this intervention generally has a favorable impact on the weight balance, the practice of sports, the clothing possibilities and the patient’s psychological state.
It is simply a matter of patience. You will have to wait the time needed for the scars to reduce. You will also have to carefully monitor the scarring evolution and consult about every three months during the first year. The operated breast is a breast that remains natural and sensitive, in particular to the hormonal and weight variations.
The purpose of this cosmetic surgery is to bring improvement and not to achieve perfection. If your wishes are realistic, the result should give you great satisfaction.
IMPERFECTIONS
The scars, which are carefully monitored, appear pink and swollen in the second and third postoperative months. Beyond that, they generally fade gradually to become, with time, slightly visible. They may however be larger than expected, white or brown.
As far as scars are concerned, it should be known that, if they generally fade over time, they cannot completely disappear. In this respect, it should not be forgotten that if the sutures depend on the surgeon’s performance, the scar, depends on the patient.
Sometimes, breast asymmetry may persist in volume, height, size or orientation of the areola.
In all cases, a secondary surgical correction can be performed, but should be scheduled at least a year or two of the first procedure.
THE POSSIBLE COMPLICATIONS
Although essentially carried out for aesthetic motivations, a mastopexy remains a true surgical act, which implies risks associated with any medical act, however minimal they may be.
The postoperative follow-ups of a breast lift are generally simple. However, complications may occur, some of them inherent to any surgical operation, others more specific to the treatment of breast ptosis.
The complications associated with anesthesia must be distinguished from those related to the surgical procedure:
- Regarding the anesthesia:
During the consultation, the anesthesiologist will inform the patient about the anesthetic risks. It must be known that anesthesia induces reactions in the body that can be sometimes unpredictable, and more or less easy to control. The choice of a perfectly competent anesthesiologist working in a surgical environment implies that the risks involved are statistically negligible.
Indeed, the techniques, the anesthetic products and the monitoring methods have made tremendous progress over the last twenty years, offering optimum safety, especially when the surgical procedure is carried out on a healthy patient without any emergency.
- Regarding the surgical act:
By choosing a qualified and competent cosmetic surgeon that has been trained in this type of procedure, you minimize these risks, but do not completely eliminate them.
Fortunately, after a breast lift the real complications are rare. In practice, the vast majority of surgeries take place without any problems and the patients are fully satisfied with the result. However, despite their low frequency, you still have to know the possible complications:
- Thromboembolic incident (phlebitis, pulmonary embolism): although generally very rare after this type of intervention, thromboembolic incidents are among the most formidable. Rigorous preventive measures must be put in place to minimize their incidence: wearing anti-thrombosis stockings, an early postoperative rising and possibly anti-coagulant treatment.
- The occurrence of an infection: It requires antibiotic treatment and sometimes surgical drainage.
- A hematoma: It may require a surgical procedure.
- A delay in the scarring process: he healing of the scar can sometimes be delayed, which lengthens the postoperative follow-ups.
- Skin necrosis: rarely observed with modern techniques, a cutaneous necrosis can be responsible for a delay of the healing process. The risk is greatly increased by tobacco consumption.
- Altered sensitivity: Especially at the level of the nipples. These alterations can be observed, but the normal sensitivity reappears most often within 6 to 18 months.
- The scarring “ears”: Located at either end of the horizontal scars, they may also require surgical correction several months after surgery.
- Evolution of the scars: the occurrence of hypertrophic or even keloid scars of unpredictable appearance and evolution can compromise the aesthetic appearance of the result and require local treatments that can last long.
Thus, in the vast majority of cases, this intervention, thoroughly studied and correctly performed, gives a very appreciable result, even if the inevitable scarring result remains the main disadvantage.
CONCLUSION
One should not overestimate the risks, but simply realize that surgery, even seemingly simple, always involves a small amount of hazards.
To prevent these complications from happening and to ensure that they will be treated effectively if necessary, the choice of a qualified plastic surgeon is paramount.