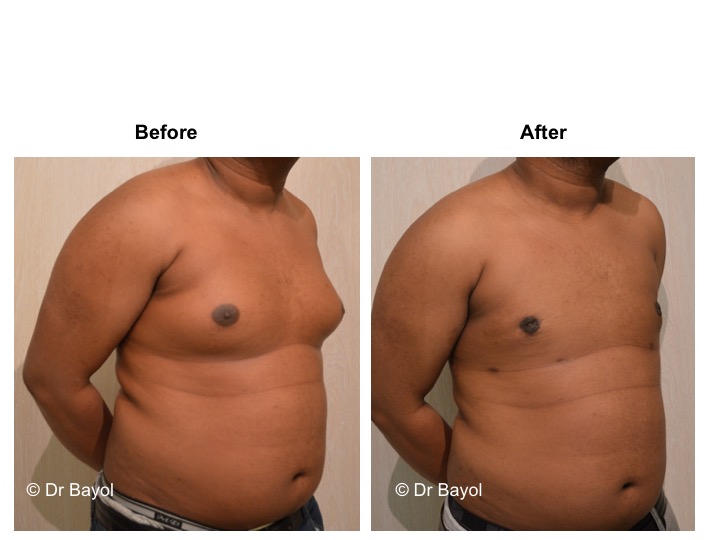
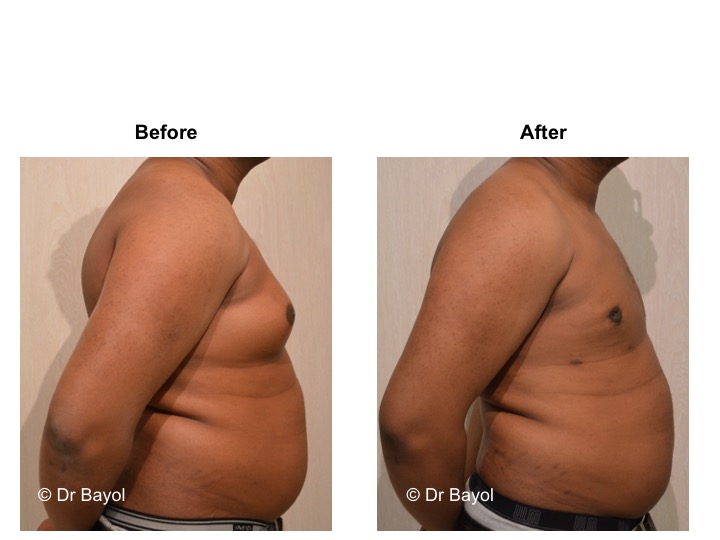
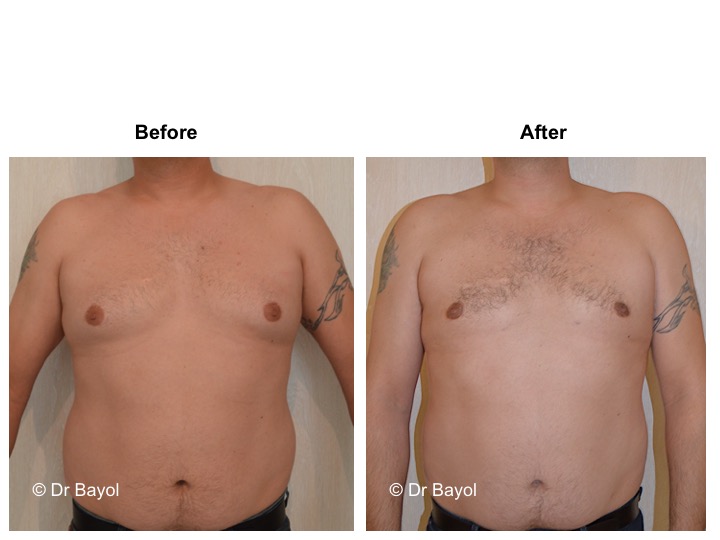
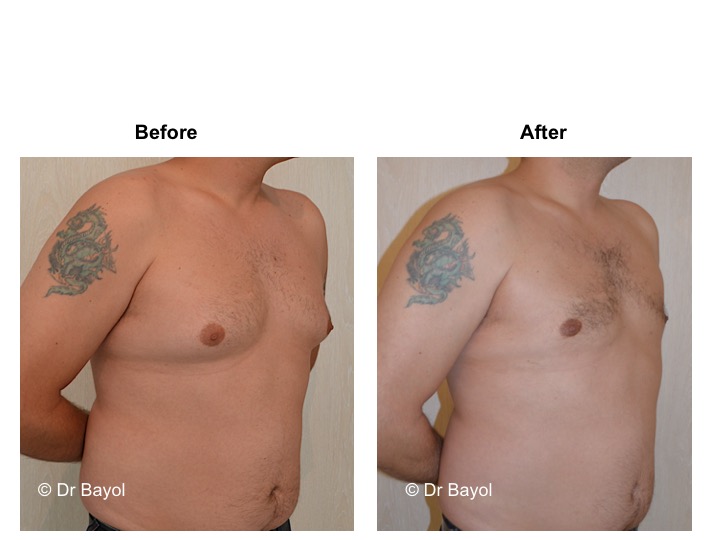
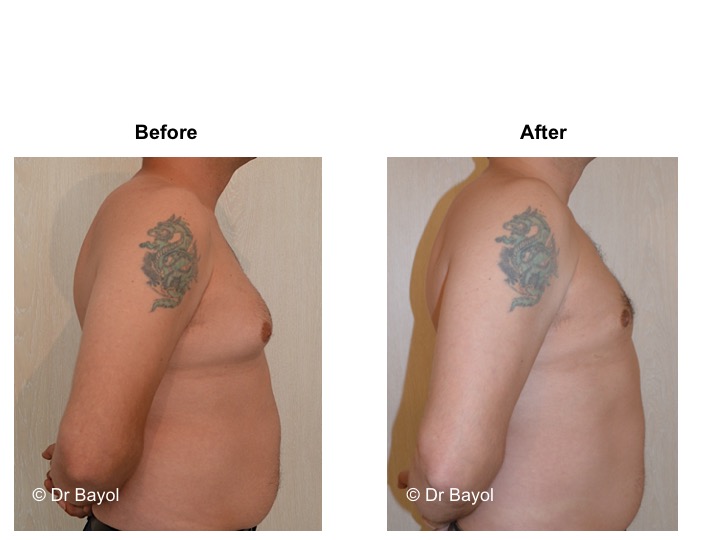
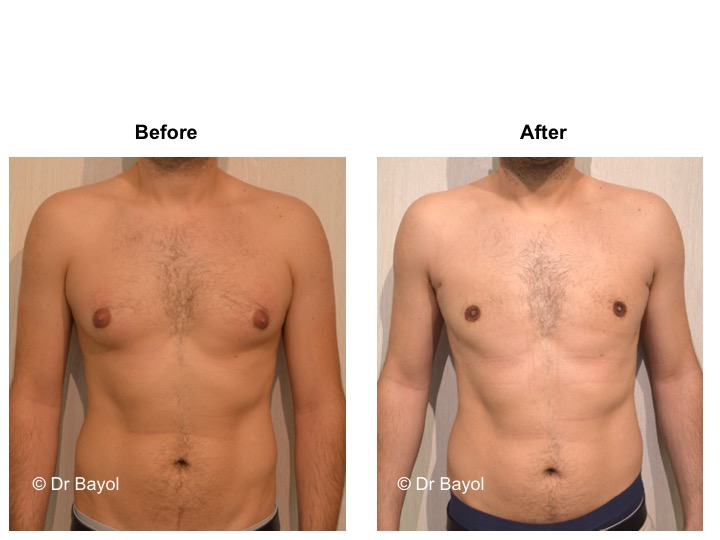
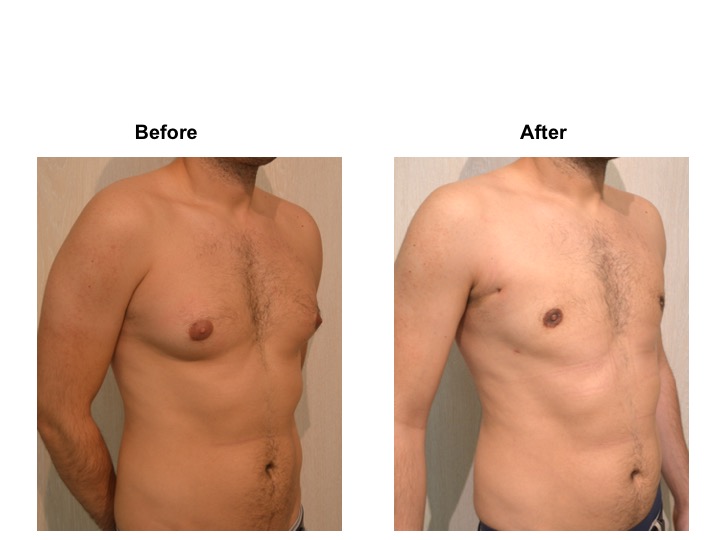
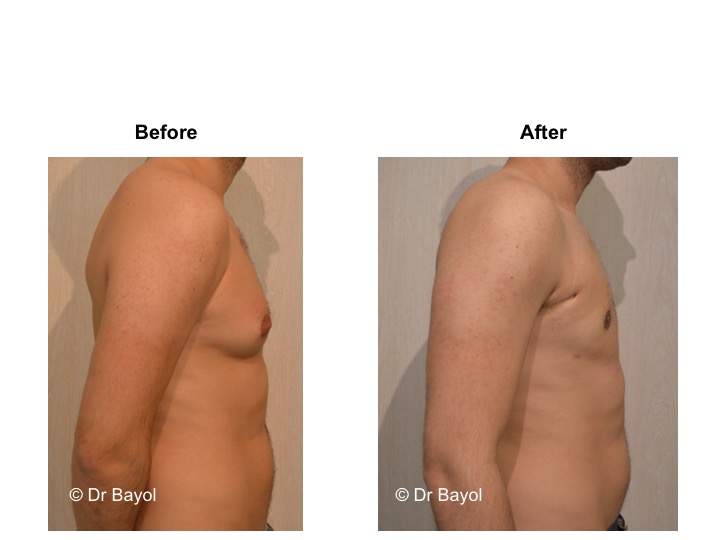
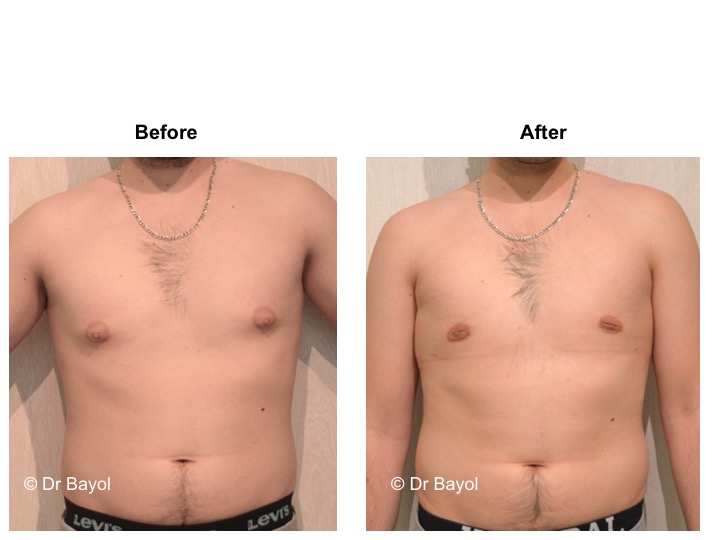
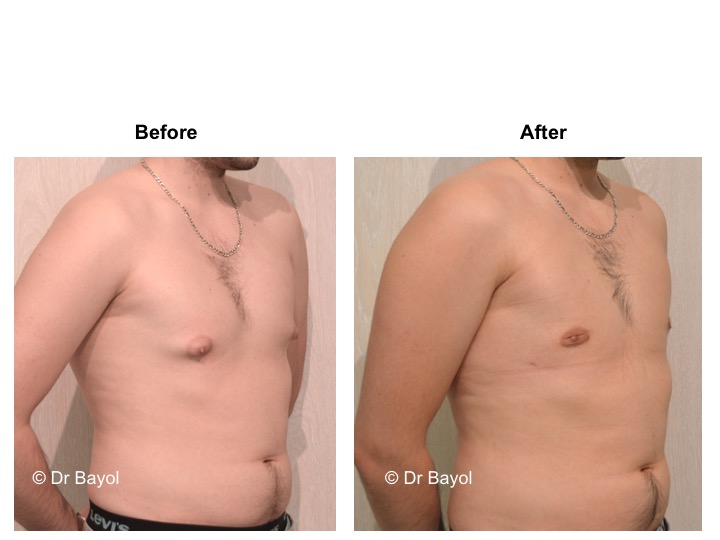
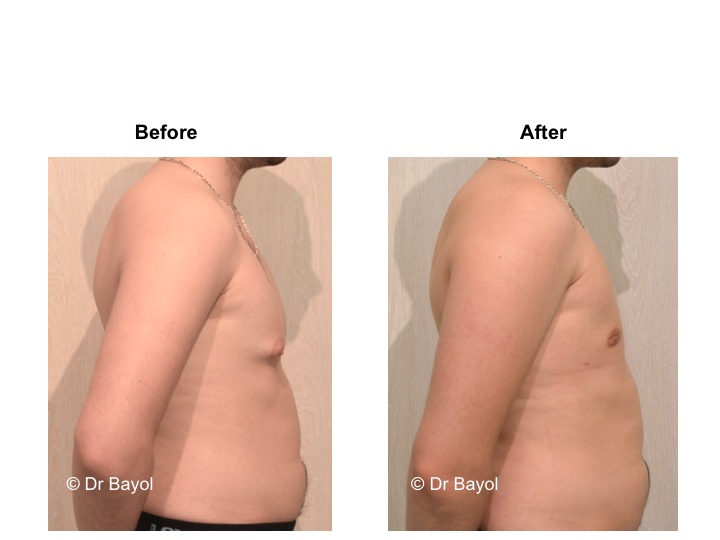
GYNECOMASTIA TREATMENT
Gynecomastia corresponds to the increase in the size of male breast tissue. Most often there is no direct cause to this phenomenon. However, it may be related to the taking of a drug, a disease, or a tumor. Gynecomastia has to be differentiated from the adipomasty, more frequent and related to overweight. In both cases, the procedure’s principle is to reduce the breast size and to remove the excess gland.
> all about GYNECOMASTIA <
GYNAECOMASTIA COSMETIC SURGERY IN MONTREUX, LAUSANNE AND GENEVA (SWITZERLAND)
A gynecomastia corresponds to an increase in the volume of the mammary gland in the man’s body. Most often, there is no cause for its occurrence. Sometimes it can be connected to an abnormal and excessive hormonal activity, or to certain medications.
Before considering any procedure of cosmetic surgery, a check-up to search the cause must be performed. Most often this assessment will include hormonal assays and radiological examinations (thoracic radiography, testicular ultrasound, mammography). This check-up will make it possible to diagnose a lesion of the lungs, a tumor of the testicle, a tumor of the pituitary gland (hormonal gland within the skull) or a breast cancer. When the cause is found, it will have to be treated. This will most often make the gynecomastia regress.
In the case of a male adolescent, an increase in breast volume causes a very important psychological discomfort, physical complexes and withdrawal. Gynecomastia can also be very painful.
It should be noted that the mammary gland is normally present in men’s body, but it is almost invisible since it is reduced to a simple mammary bud. The mammary gland can sometimes develop if the hormonal environment is conducive.
If the biological and radiological assessment does not find any cause, a cosmetic surgery can be considered. To do so it is paramount that the patient is in good physical and psychological form. This surgical procedure is called gynecomastia treatment.
CLINICAL CHARACTERISTICS OF A GYNECOMASTIA
Gynecomastia is characterized by a development of the mammary gland centered on the areola. It has the particularity of being bilateral and asymmetrical, it has of firm consistency and is sensitive to palpation.
We must distinguish a gynecomastia from an adipomastia. Adipomastia is much more frequent, it corresponds to an overload of fat localized at the level of the breast. It is often observed in cases of patients with overweight. The difference with gynecomastia is that adipomastia is not centered on the areola, it is soft, painless, bilateral and symmetrical. However, adipomastia and gynecomastia can be connected.
Gynecomastia may transiently appear in adolescents due to estrogen-related hormonal imbalance and usually disappear within a few months.
Men’s breast cancer is very rare and has a different appearance. It affects men over 40 years old. A male breast cancer occurs in the form of a unilateral, hard, insensitive lesion associated with deformations or retractions of the nipple or even bleedings.
PRINCIPLES OF THE GYNECOMASTIA CURE
The aim of the procedure is to restore the normal anatomy as best as possible with the following principles:
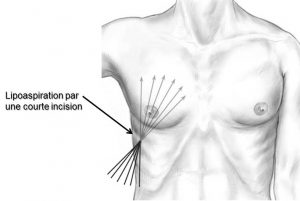
- To diminish the breast volume: Either by direct surgical resection of the mammary gland (subcutaneous mastectomy), or by liposuction of the fat. In the case of an associated form, both techniques will be used.
- To reduce the excess skin: most often, the reduction of the glandular volume will allow the retraction of the skin. The liposuction will favor this retraction which will be effective since it is a young man with a good quality of skin. Postoperative massage may also help with skin retraction. However, when the excess skin is too great, a breast reduction will have to be performed and will leave scars. This cutaneous mammary reduction can be carried out during the first or the second procedure.
BEFORE THE SURGICAL INTERVENTION
The preoperative check-up has been mentioned previously. This assessment will be prescribed by your treating physician or an endocrinologist. Doctor Jean-Charles BAYOL will also be able to prescribe this assessment after your first appointment at Laclinic-Montreux, or at the Beauty Suite in Lausanne, (only 30 minutes from Geneva).
In case of significant overweight, a diet associated with physical exercises is necessary, as a loss of weight can cause gynecomastia to decrease or even disappear (mainly due to an adipomastia).
Depending on the anatomical conditions and the wishes of the patient, a surgical strategy will be decided in order to obtain the best result. Dr. Jean-Charles BAYOL will discuss with his patient the surgical technique that will be used and the location of the future scars (see “gynecomastia treatment”).
A preoperative blood test will be performed and you will meet the anesthesiologist, no later than 48 hours before surgery. It will be imperative to communicate your medical treatments in progress to the surgeon but also to the anesthesiologist. Indeed, some treatments may interfere with the anesthesia or promote bleeding.
Medications containing aspirin or anti-inflammatories should be prohibited within ten days before surgery (because they promote bleeding).
It is recommended to stop smoking at least one month before and one month after surgery, as tobacco may delay the healing process.
ANESTHESIA AND HOSPITALIZATION FOR A GYNECOMASTIA TREATMENT
The procedure is usually performed under general anesthesia, during which the patient is in a deep sleep. In some cases, a thorough local anesthesia with intravenous tranquilizers (conscious anesthesia) or a simple local anesthesia may be used (this will need to be be discussed with the surgeon and the anesthetist).
The treatment of gynecomastia is most often performed as an outpatient surgery. This is a one-day hospitalization at Laclinic in Montreux, with a check-out in the evening after a few hours of postoperative monitoring.
SURGICAL INTERVENTION: THE CURE OF GYNECOMASTIE
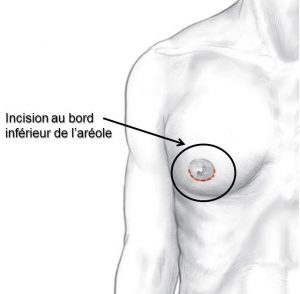
An incision is made on the lower edge of the areola
Usually, it is a lower hemi-periareolar scar (Figure 1). Through the incision, the gland can be removed. This procedure will often be associated with a liposuction (lien vers “liposuccion”) of the chest at the periphery of the glandular excess in order to harmonize the result.
Figure 1: Lower areolar scar made during the treatment of gynecomastia
In the case of an isolated or predominant adipomastia, only liposuction is performed. The scars are then very short and can be located in the under-mammary or axillary regions (Figure 2).
In cases with important cutaneous excesses, the plastic surgeon may have to make longer and more visible scars. These scars can be horizontal and extended on either side of the areola (the nipple). In some extreme cases the surgeon will graft the areola and the nipple. Other types of scars are possible (vertical, racquet-shaped) and depend on each particular case.
At the end of the surgical procedure a drain is placed on each side to eliminate blood and lymph residues that could accumulate around the scar and cause a hematoma.
After the dressing has been made, a compressive elastic garment is put in place.
The duration of the intervention varies depending on the cosmetic surgeon and the technique used. Usually the procedure lasts one to two hours.
AFTER THE CURE OF GYNECOMASTIE
The postoperative pain is usually moderate, in all cases an analgesic treatment will be prescribed. Regarding the immediate postoperative outcomes, bruises (ecchymoses) and swelling (edema) are the most common. These marks can be more or less important and may descend on the belly.
In order to limit the importance and the duration of these outcomes, you will be systematically taken care of by the department of physiotherapy for postoperative care. On the same day, gentle massages of the operated area and LED care will ensure lymphatic drainage and will facilitate the healing process. Several weeks after the procedure, a LPG treatment can be undertaken.
Simple daily dressings should be performed for a period of 10 to 15 days.
An elastic restraining vest, promoting cutaneous retraction, must be worn for 6 weeks.
A leave period will have to be scheduled for 7 to 10 days after the procedure.
It will take between 4 and 6 weeks to resume a sporting activity.
THE SCARS OF THE GYNECOMASTIA TREATMENT
A scar is a surgical stigma. The goal of the cosmetic surgeon is to make the “best” scar possible.
The time it takes for a scar to evolve is one to two years. The scar is thin and white in the first month, then it becomes pink, even red and indurated until the sixth month. This second phase of the scar evolution can be much longer. Finally, they gradually bleach. It is essential to protect the scar from the sun for 6 to 12 months.
The length and the position of the scar vary according to the surgical technique that has been used. The quality of the scar depends on the surgical technique and also on factors specific to the patient (age, quality and type of skin …).
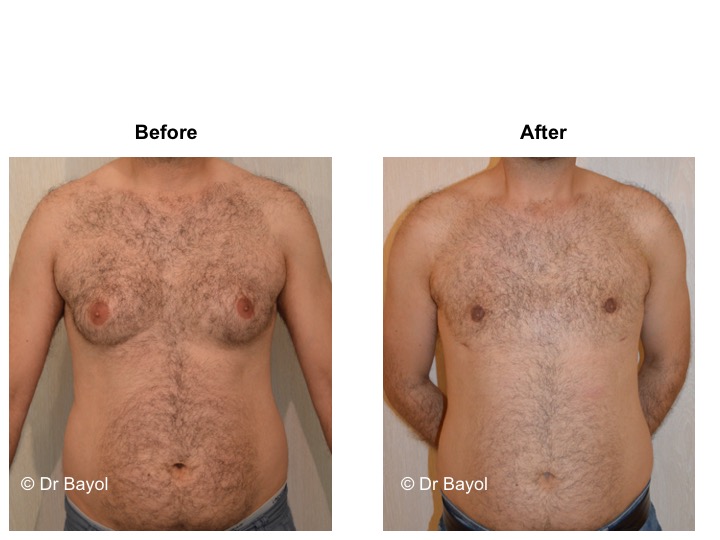
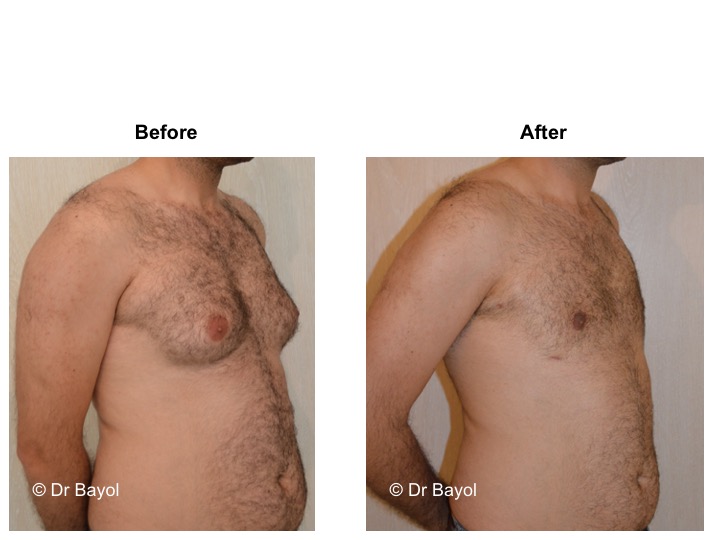
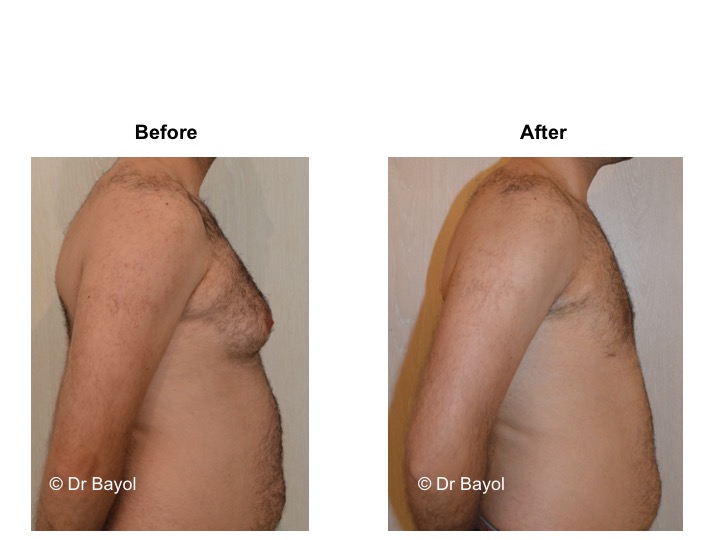
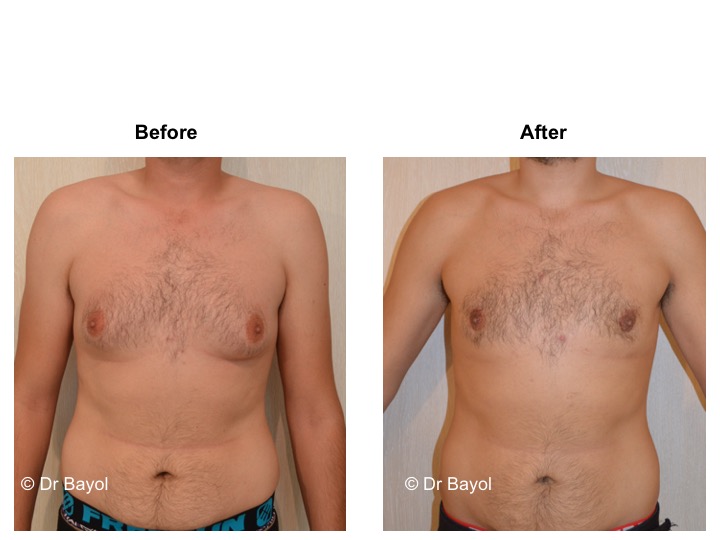
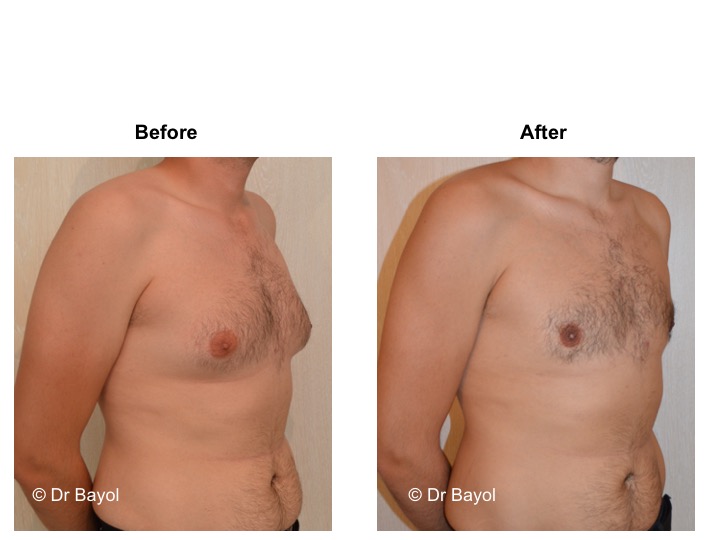
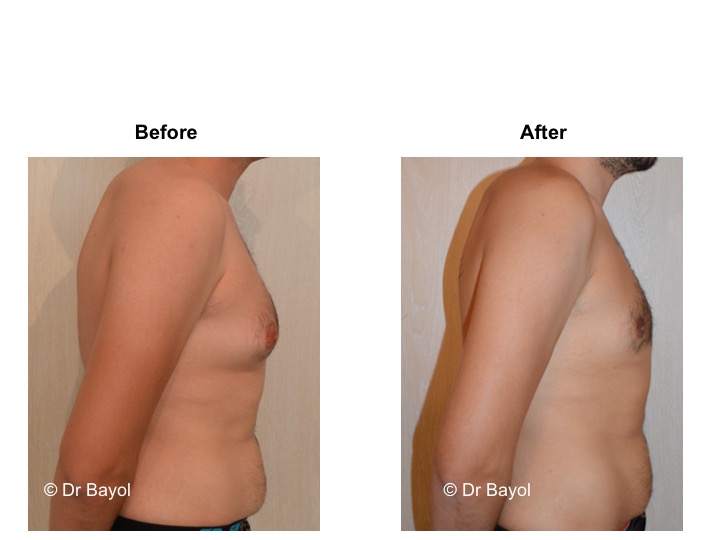
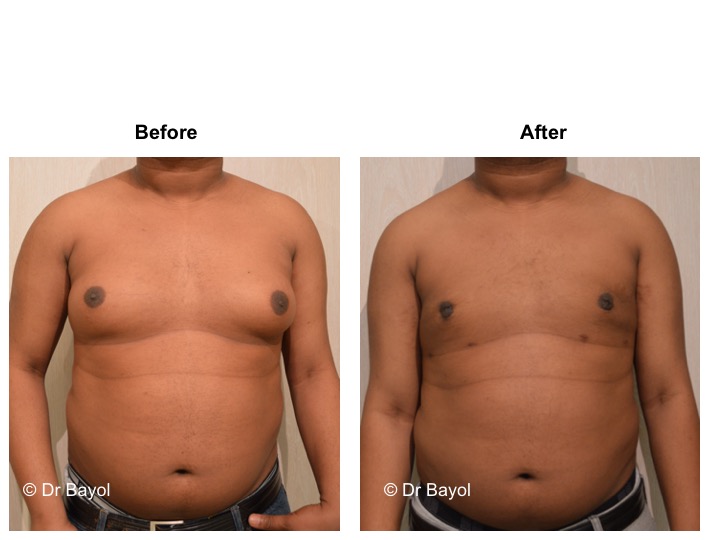
RESULT OF COSMETIC GYNECOMASTIA SURGERY IN MONTREUX, LAUSANNE AND GENEVA (SWITZERLAND)
The aesthetic improvement is usually clear and immediate. However, it takes 3 to 6 months to estimate the final result. This period corresponds to the time it takes for the edema to disappear and the skin to retract. Beyond the sixth month the tissues will gradually soften.
The reduction in the volume of the breast brings physical comfort to the patient, especially during dressing and undressing. The result of the surgical procedure is very beneficial, especially on a psychological level since gynecomastia deeply disturbs the patient’s manhood.
When gynecomastia is predominantly glandular, the result will be stable in the long term and recurrence will not occur. When gynecomastia is associated with a fat overload (adipomastia), any gain of weight will cause a new increase in breast volume. Hence the fundamental importance of maintaining a stable weight or even lose weight after the procedure.
RESULT’S IMPERFECTIONS
- Asymmetry: due to lesser excision on one side than on the other, especially when there was already an asymmetry of volume before the intervention. Most often, it diminishes with the wearing of compressive dressing, massages and time can also help the healing process. If it persists a correction can be performed.
- Difference of size or position of the nipples: most often this difference exists before the procedure. Dr. Jean-Charles BAYOL always draws the attention of his patients on these pre-existing symmetries, before the surgical act.
- Cupulation of the areola: it is most often due to an excision of the gland located behind the areola without a harmonious excrescence of the outskirt. If it is bothersome and persistent, it can be retouched surgically.
- Excess of skin: in the case of an important gynecomastia, the excess of residual skin may take several months to retract. The retraction depends on the skin quality.
- Recessed areas and / or small nodules under the skin: due to liposuction which can sometimes aggravate the appearance of cellulite. This is a normal phenomenon, massage sessions will allow to split these fibrous nodules and avoid their adhesions.
The sensitivity of the nipples is not altered by the procedure but can be transient for a few months. The insensitivity is exceptional. However, if the surgeon needs to graft the nipple (see chapter surgical intervention), the insensitivity may become permanent and result in a discoloration (dyschromia).
POSSIBLE COMPLICATIONS OF THE GYNECOMASTIA
Although essentially performed for psychological and aesthetic motivations, the treatment of gynecomastia remains a true surgical act which implies risks associated with any surgical operation, however minimal they may be.
After a gynecomastia, the postoperative follow-ups are generally simple. However, complications may occur, some of them inherent to any surgical operation, others more specific to this intervention.
-The complications related to anesthesia:
It is the anesthetist who will inform you about complications related to anesthesia, during the preoperative consultation.
The choice of a competent anesthetist working in a surgical clinic lowers the risks significantly.
Indeed, the techniques related to anesthesia have considerably improved over the last thirty years, allowing an optimal safety, especially when the procedure is performed on a healthy person without any emergency.
-The complications related to the surgical gesture:
By choosing a qualified and competent cosmetic surgeon trained in this type of procedure, you will considerably limit these risks, without completely removing them, however.
Most of the gynecomastia treatments are carried out according to the rules and without any complication. The postoperative follow-up is smooth and patients are fully satisfied with the outcome of the procedure.
However, complications exist and must be known:
- Postoperative hematoma: it can occur within hours after surgery. If it is voluminous, it will require a surgical correction to suppress it.
- Thromboembolic complications, phlebitis and pulmonary embolism: these complications will be prevented by the wearing of stockings for two weeks after surgery, a swift resumption of walking can also help.
- Lymphocele or seroma: an effusion of the lymphatic fluid in the zone of detachment is possible. This effusion may require one or more punctures to drain it.
- Infection: it can occur at the end of the procedure. The infection results in a swollen, red and painful breast, generally accompanied by a fever. Antibiotic treatment may be sufficient, but surgical drainage may be sometimes required.
- Skin necrosis: it is very rare and favored by a poor cutaneous vascularization, mainly caused by tobacco consumption. Hence smoking at least 6 weeks before the procedure should be prohibited. When cutaneous necrosis occurs, it will be treated with local dressings. The scarring process will be achieved but with a slight delay.
- Pneumothorax: very rare, a specific treatment will be needed.
- Pathological scars: Even if the surgeon uses all his art to make fine and discreet scars, the process of scarring varies with each patient. Indeed, scarring is a random phenomenon and sometimes the scars may not be as discreet as desired. For the same individual, depending on the regions of the body, the healing process may be variable. Thus, the scarring evolution may not be as expected with the appearance of hypertrophic or even keloid scars whose evolution is unpredictable. These pathological scars can compromise the aesthetic appearance of the result and require local treatments that are often long.
- Troubles regarding cutaneous sensitivities: as we have seen in the chapter “imperfection of the results”, these disorders are transient but can last several weeks. On the other hand, in the case of a grafting of the areola-nipple plaque, the insensitivity may be permanent.
CONCLUSION
The treatment of gynecomastia brings a real aesthetic and psychological benefit to the patient.
The result of this procedure is most often rapid and spectacular.
Complications are rare and risks should not be overestimated. One must just understand that a surgical procedure, even simple, always involves a small amount of hazards.
To prevent these complications from happening and to ensure that they will be treated effectively if necessary, the choice of a qualified plastic surgeon is paramount.